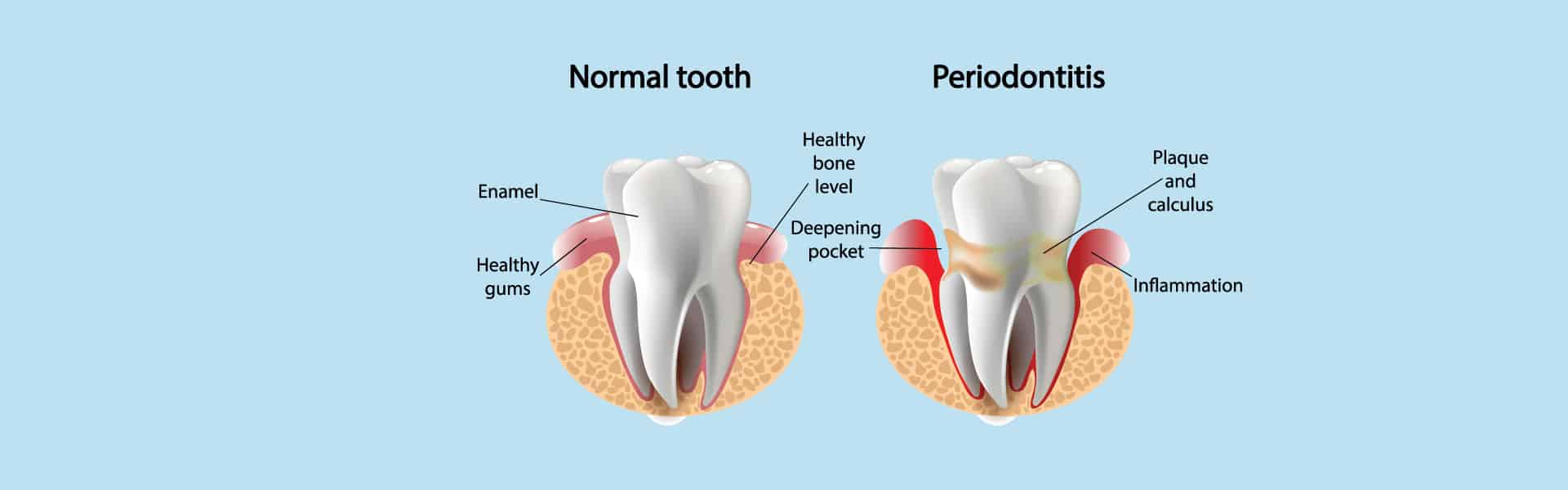
Periodontal Disease
You probably learned to clean your teeth when you were a child. The techniques and tools that were effective then are not sufficient to maintain your teeth and gums now that they have been damaged by periodontal disease.
In a healthy mouth, the space between the tooth and gums (called the sulcus) is normally only two to three millimeters deep. It’s not difficult to clean that at home with careful brushing. But when you have periodontal disease, the sulcus deepens, forming pockets around your teeth. These are deeper than three millimeters, so they’re notorious hiding places for plaque and disease-causing bacteria.
Another problem when you have periodontal disease has to do with the shape of the roots of your teeth. If there is no periodontal disease, the bone level is high and the gums attach firmly at the necks of the teeth. You can easily wrap floss around this surface and do a thorough job of keeping plaque off your teeth.
Swollen Gums from Periodontal DiseaseBut periodontal disease decreases the attachment of the bone and gums to your teeth. The root surfaces are often exposed, and they have small indentations in them. Floss glides over these indentations, missing the plaque hiding inside.
You need to use special tools to reach down beyond the normal three millimeters to thoroughly clean the indentations in the sides of the roots. There are tools made specifically for each area of your mouth. We will work with you to customize a plaque-removal system and teach you how to use that system at home.
Periodontal disease is an infection of the teeth and gums, as well as the bone that surrounds the teeth. If left untreated, it causes supporting bone to be lost from around the teeth. Periodontal disease is the number-one cause of tooth loss in the United States today. There are three stages to periodontal disease-gingivitis, periodontitis, and advanced periodontitis.
Plaque, a sticky film of food and bacteria, forms constantly on teeth. If it isn’t removed daily, it begins to harden and forms tartar (calculus). In this early stage, before bone loss has occurred, the gums become red and swollen; this is gingivitis.
Periodontal Disease X-RayAs the plaque and tartar work their way down below the gum line, the gums begin to separate away from the teeth, forming pockets. Once a pocket has formed, the process accelerates, as new, even more destructive types of bacteria begin to populate the pocket. If the tartar isn’t removed by dental professionals, your body’s defensive reaction to the infection produces enzymes that cause the loss of supporting bone; this is periodontitis.
Over time, if periodontitis continues unchecked, this bone loss continues. Eventually, so much bone is lost that some of the teeth begin to become loose. This is advanced periodontitis.
Routine cleanings in our office remove plaque and tartar that exist on your teeth above the gumline, But sometimes, especially if you don’t floss regularly, plaque, tartar and bacterial toxins can develop below the gumline where your toothbrush can’t reach. The goal of scaling and root planing is to eliminate this source of periodontal infection from below the gumline, at the surfaces of the roots. The procedure
Normally, we’ll spread a scaling and root planing procedure out over several appointments. This allows us to check on the healing and help you fine-tune your home care efforts.
To keep you comfortable, we will give you a local anesthetic before the procedure begins. Once you’re completely numb, we’ll use either a small scaling instrument or an ultrasonic cleaner to get rid of all plaque and tartar, from the top of your tooth all the way down to the bottom of the pocket.
Then, we’ll plane – or smooth – your tooth so your gums can heal and reattach to your teeth. If it appears to be necessary, a small antibiotic fiber will be placed into the pocket area after it’s been scaled and planed to control infection and promote healing. Antibiotics might also be prescribed to further combat the infection. Once the source of infection has been removed, your gums will begin to heal, and will once again tighten around your teeth.
Maintaining Periodontal Health
Homecare is the key to continuing the healing process. Since brushing and flossing only clean about three millimeters below the gumline, you’ll need special tools to clean the infected areas. As part of your treatment, we’ll provide you with the tools and techniques you’ll need to thoroughly clean these transitional areas.
Having diabetes puts you at higher risk for oral infections and gum disease (also called periodontal disease). Why? Because diabetes weakens your mouth’s natural ability to fight off germs, including the plaque bacteria that cause gum disease.
Harmful bacteria in your mouth thrive on glucose, the kind of sugar that’s linked to diabetes. When diabetes isn’t properly controlled, high glucose levels in the mouth promote the growth of this bacteria and can lead to tooth decay and periodontal disease, according to the American Diabetes Association. Diabetics may also experience diminished salivary flow, which also contributes to tooth decay by drying out the mouth.
A lack of moisture in the mouth allows plaque – the sticky film of food residue and bacteria – to build up on your teeth, leading to a greater chance of tooth decay and periodontal disease.
Smoking Worsens the Problem!
If you’re a smoker over age 45, and you have diabetes, you are at 20 times greater risk of having gum disease, because smoking further diminishes your body’s natural ability to heal itself.
Gum disease is not to be taken lightly. In its advanced stages, gum disease has been linked to serious health problems like heart disease, stroke and premature or low-weight babies. Gum disease can also cause you to lose your teeth, and it will worsen your diabetes.
Sign That You May Have Periodontal Disease
- Gums that bleed when you brush or floss
- Gums that are red, swollen and/or tender
- Gums that have pulled away from your teeth
- Bad breath or a bad taste in your mouth that won’t go away
- Pus between your teeth and gums when you press on that area
- Permanent teeth that feel loose
- Teeth that don’t line up like they did in the past
Heart Disease and Periodontal Disease
Recent studies have shown that individuals with severe gum disease are four times more likely to suffer from coronary heart disease.
Researchers at the University of Minnesota in Minneapolis recently discovered that this chronic infection in your mouth creates an open doorway for plaque bacteria to enter the bloodstream. These bacteria, called streptococcus sanguis, may cause blood clots that can block your arteries and even trigger a heart attack.
Other studies have shown that plaque bacteria entering the bloodstream through infected gums may also cause a potentially fatal heart disease called infective endocarditis. This is a bacterial infection which causes the sac around the heart to become inflamed.
How you can reduce your risk
Regular dental exams can reduce your risk of heart disease and stroke. So do your heart a favor. Brush, floss, and visit us twice a year for a checkup and cleaning!
Diabetes and Periodontal Disease
You will need to be diligent about your oral hygiene, brushing and flossing daily and seeing us at least twice a year for an exam and a professional cleaning. You will also need to have your triglyceride and cholesterol levels checked regularly; these factors have also shown a direct correlation to the development of gum disease.
Respiratory Infections
An open door to infection, Plaque, a sticky film of food and bacteria, forms constantly on your teeth. If it isn’t removed daily, it begins to harden and forms tartar (calculus). In this early stage, before bone loss has occurred, the gums become red and swollen; this is gingivitis. As the bacteria in plaque and tartar work their way down below the gum line, the gums begin to separate away from the teeth, forming pockets. Once a pocket has formed, the process accelerates as new, even more destructive types of bacteria begin to populate the pocket. If the calculus isn’t removed by dental professionals, the defensive reaction by your body produces enzymes that cause the loss of supporting bone; this is periodontitis. Over time, if periodontitis continues unchecked, the bacterial infection spreads throughout your mouth, and bone loss accelerates.
As you breathe in normally, the bacteria in your gums can transfer to your lungs, where they breed and multiply. It is now thought that the bacteria in your lungs can develop into respiratory infections such as pneumonia, bronchitis, emphysema, and chronic obstructive pulmonary disease.
Prevention and treatment of periodontal disease lowers your risk of respiratory infection!
You can minimize your risk of periodontal disease, and respiratory infections, by following a dental hygiene discipline that includes brushing twice daily, flossing at least once a day, and visiting us twice a year for dental cleanings. We also recommend that you avoid smoking, eat a balanced diet, and maintain a generally healthy lifestyle, as periodontal disease has been linked to other medical conditions, including heart disease and uncontrolled diabetes.
Prompt treatment of periodontal disease removes the source of bacteria, allows your gums to heal, and stops the progressive loss of bone. The added bonus? You’ll boost your overall health and decrease your risk of respiratory infections.
Infective Endocarditis(Heart Infection)
Infective endocarditis is a rare, life-threatening disease that inflames the interior lining of your heart. Bacteria from plaque called Streptococcus Sanguis cause the disease when they enter your bloodstream and adhere to damaged heart tissues or valves. Because infective endocarditis is such a serious condition, prevention is vital.
Gums infected with periodontal disease are reservoirs of disease-causing bacteria. The bacteria reside in pockets next to the teeth where the diseased gums have pulled away from the tooth surface. When your gums bleed, a doorway is created for the plaque bacteria to travel from your mouth into your bloodstream, potentially infecting other areas of your body.
The American Dental Association and the American Heart Association recommend that you take antibiotics before dental treatment if your physician has told that you are at risk for developing Infective Endocarditis, or if your medical history includes:
- Valvular Heart Disease
- A congenital heart defect
- Mitral Valve Prolapse
- Rheumatic Heart Disease
- An artificial heart valve
- Intravenous drug use
When you make your appointment for dental treatment, especially for procedures that may cause your gums to bleed, we’ll evaluate your medical history to see if you are at risk for infective endocarditis. We must also know whether you are allergic to any drugs or if you are currently taking medication. If endocarditis is a concern, we will prescribe the appropriate antibiotic and give you instructions for the frequency and dosage.
In order to protect your heart, it’s crucial that you avoid periodontal disease by keeping your teeth and gums free of plaque and tartar (calculus). Brush thoroughly after each meal, floss each and every day, and keep your regular dental visits for cleanings and continued homecare evaluation and instructions.
Periodontal Disease and Pregnancy
Mothers with severe periodontal disease are seven times more likely to deliver pre-term, low-birthweight babies, according to a study of 124 pregnant women conducted at the University of North Carolina and published in 1996 in the Journal of Periodontology
Scientists think this link is due to the body’s reaction to the bacteria in gums infected with periodontitis When you have periodontal disease, bacterial toxins attack the bone, ligaments and gums that surround your teeth. You essentially have a large open wound in your mouth that creates a doorway for bacteria to enter your body through your bloodstream.
One of your body’s reactions to this infection is to produce more prostaglandins, which cause tissues to swell in response to the infection. During pregnancy, prostaglandin production rises gradually, ultimately peaking to induce labor. If you are producing extra prostaglandins in response to an infection in your gums, your body might interpret this as a signal to go into labor, and you could deliver your baby pre-term.
Researchers caution that periodontal disease does not necessarily cause early labor or low-birthweight babies, but evidence suggests that 18 percent of all low-birthweight deliveries could be attributable to periodontal disease.
Pre-term, low-birthweight babies aren’t as healthy as they could be. Complications caused by early delivery or low birthweight account for 60 percent of infant deaths.So if you’re pregnant, or thinking of becoming pregnant, there’snever been a more important time to pay attention to your oral health.
Vitamin C and Healthy Gums
Maintaining Dental Health
If you have tender, swollen gums that bleed when you brush or floss, your diet may be to blame. A study published in the August 2000 issue of the Journal of Periodontology found that people who don’t get at least 60 milligrams of vitamin C per day (the minimum daily amount recommended for adults over age fifteen) have higher rates of periodontal disease than those who get less than this amount.
In another study, to measure the effects of vitamin C deficiency on gum health, researchers at the University of California San Francisco School of Dentistry fed eleven men rotating diets for fourteen weeks. The diet purposely excluded all fruits and vegetables, which are typically high in vitamin C. During some weeks, the men were given a vitamin C supplement dissolved in grape juice. At the end of the study, researchers found that the men’s gums bled more during the weeks that they received no vitamin C. When they received the vitamin C supplement, their gums bled less.
How does vitamin C help to keep your gums healthy?
Simply put, your body needs adequate vitamin C to strengthen your bones and blood vessels, to anchor your teeth into your gums, and to form the intracellular cement your body needs for growth, tissue repair and wound healing. Vitamin C can also strengthen weakened gum tissue and make it more resistant to penetration by disease-causing bacteria.
When your gums bleed when you brush or floss, and are irritated, tender, swollen or red, you may have early gum disease, called gingivitis. This is caused by food particles and bacteria left on your teeth combining to form plaque, which hardens on your teeth and becomes tartar (also called calculus). The bacteria in plaque infect your gums, and cause them to pull back and away from your teeth (recede), forming pockets where even more bacteria can hide and reproduce. If it’s not taken care of, this infection starts attacking the roots of your teeth and the bone in your jaw, causing irreversible damage which can lead to bone loss.
Foods high in vitamin C
Many fruits and vegetables are great sources of vitamin C, but since exposure to oxygen destroys vitamin C in foods, it’s important that you eat them soon after they’ve been cut open. For example, a sliced cantaloupe left uncovered in the refrigerator loses 35 percent of its vitamin C in less than twenty-four hours.
Following are foods that are high in vitamin C:
- red and green peppers
- guavas, papayas and mangoes
- broccoli, red cabbage and cauliflower
- strawberries and raspberries
- spinach and tomatoes
- oysters
- soybeans
- cantaloupe and honeydew
Comments are closed.
